41 e/m coding guidelines worksheet
Tools and Worksheets. The following tools related to Inpatient Psychiatric Facility Prospective Payment System (PPS) are now available in the Downloads section below: Addendum A, showing IPF PPS payment updates. B Addenda, showing changes to IPF PPS ICD-10-CM/PCS comorbidity or code first codes, or lists of all IPF PPS ICD-10-CM/PCS comorbidity ...
CMS Notice Regarding Split (or Shared) Evaluation and Management Visits and Critical Care Services from May 25, 2021 through December 31, 2021. This page contains guidance regarding documentation and payment under the Medicare Physician Fee Schedule for evaluation and management (E/M) visits.
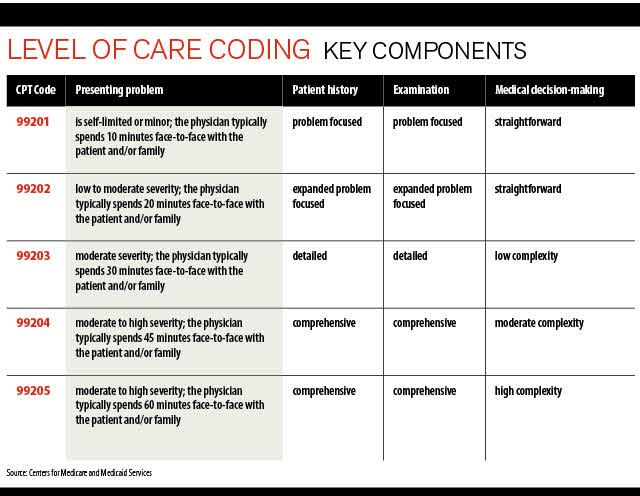
Practices have not seen many revisions to the Evaluation and Management (E/M) office / outpatient visit guidelines in three decades - until now. As of January 1, there are new E/M coding guidelines. We'll get to those in a bit, but first let's look at why they changed. Coding Tip: Understanding and Reporting Pseudoseizures.
E/m coding guidelines worksheet
E/M Coding Education, EM evaluation and management coding, e&m documentation, 99214, 99213. Web-Based E/M Coding Courses. Peter R. Jensen MD, CPC. Our E/M coding and documentation courses are designed and narrated by Peter R. Jensen, MD, CPC, founder of E/M University. Dr. Jensen is a practicing physician as well as a certified professional coder.
The full document takes the form of a new entry to CPT 2021's Errata and Technical Corrections, though the revisions to the E/M guidelines for office/outpatient codes (99202-99215) are unusually extensive. They focus on the sections that alter the scoring of medical decision-making (MDM) from the longstanding 1995/1997 guidelines.
E/M Whitepaper. E/M guidelines are undergoing enormous change as of January 1, 2021 - and all outpatient and office facilities need to be in full compliance. As the country's leader in healthcare training, we offer customized E/M Guideline training so that you'll be ready for the biggest change in medical coding since 1997.
E/m coding guidelines worksheet.
Start today with an analysis of your current E&M template. Assess what may need to be added or revised to capture the information outlined in the 2021 guidelines efficiently. Education for all providers and coders is essential for success in using this new E&M model. Stay tuned for any additional updates or clarifications.
Beginning January 1, 2021, only a " medically appropriate history and/or examination " will be required for all office/outpatient E/M codes. The number of body systems/areas reviewed and examined need only be performed and documented when medically necessary and clinically appropriate.
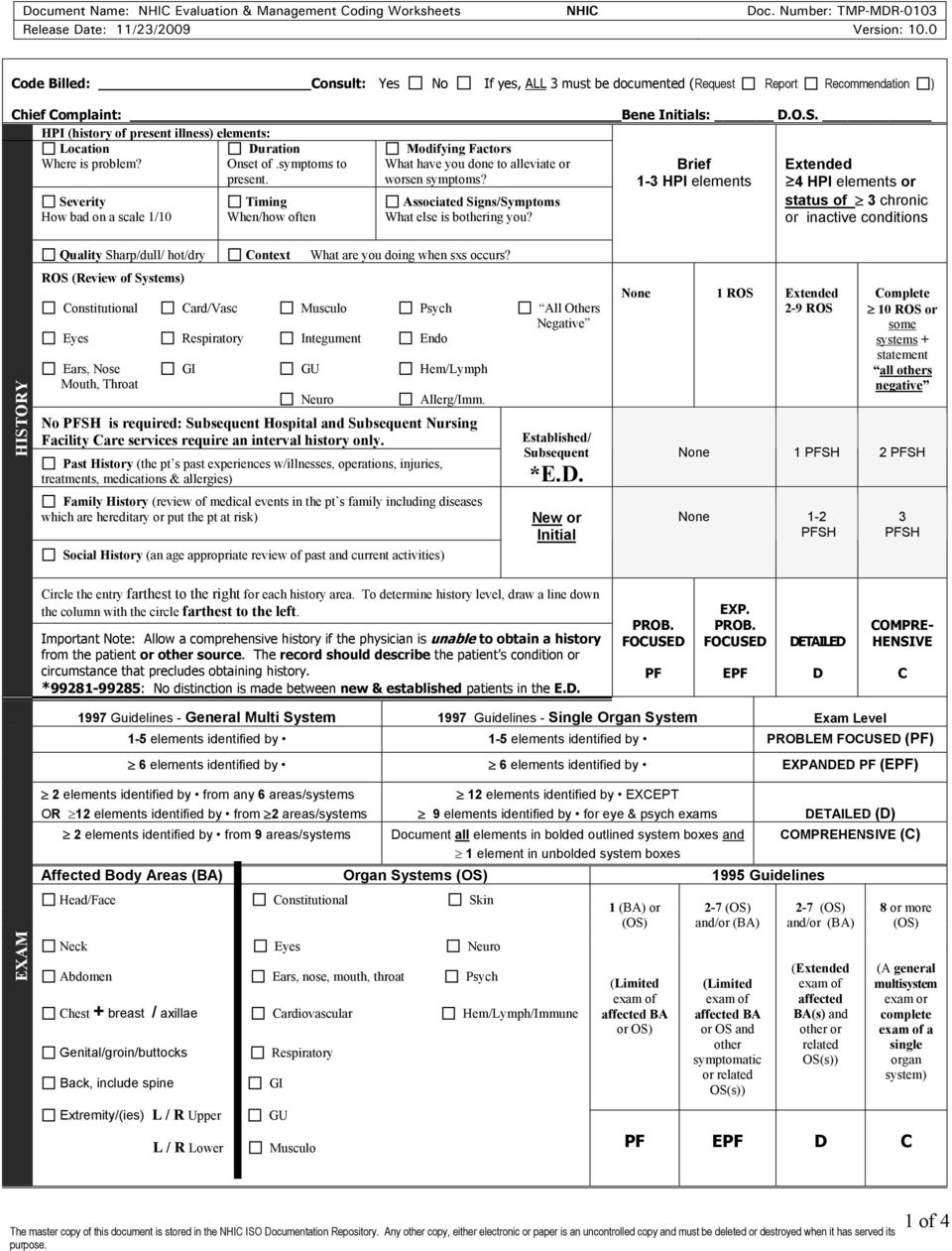
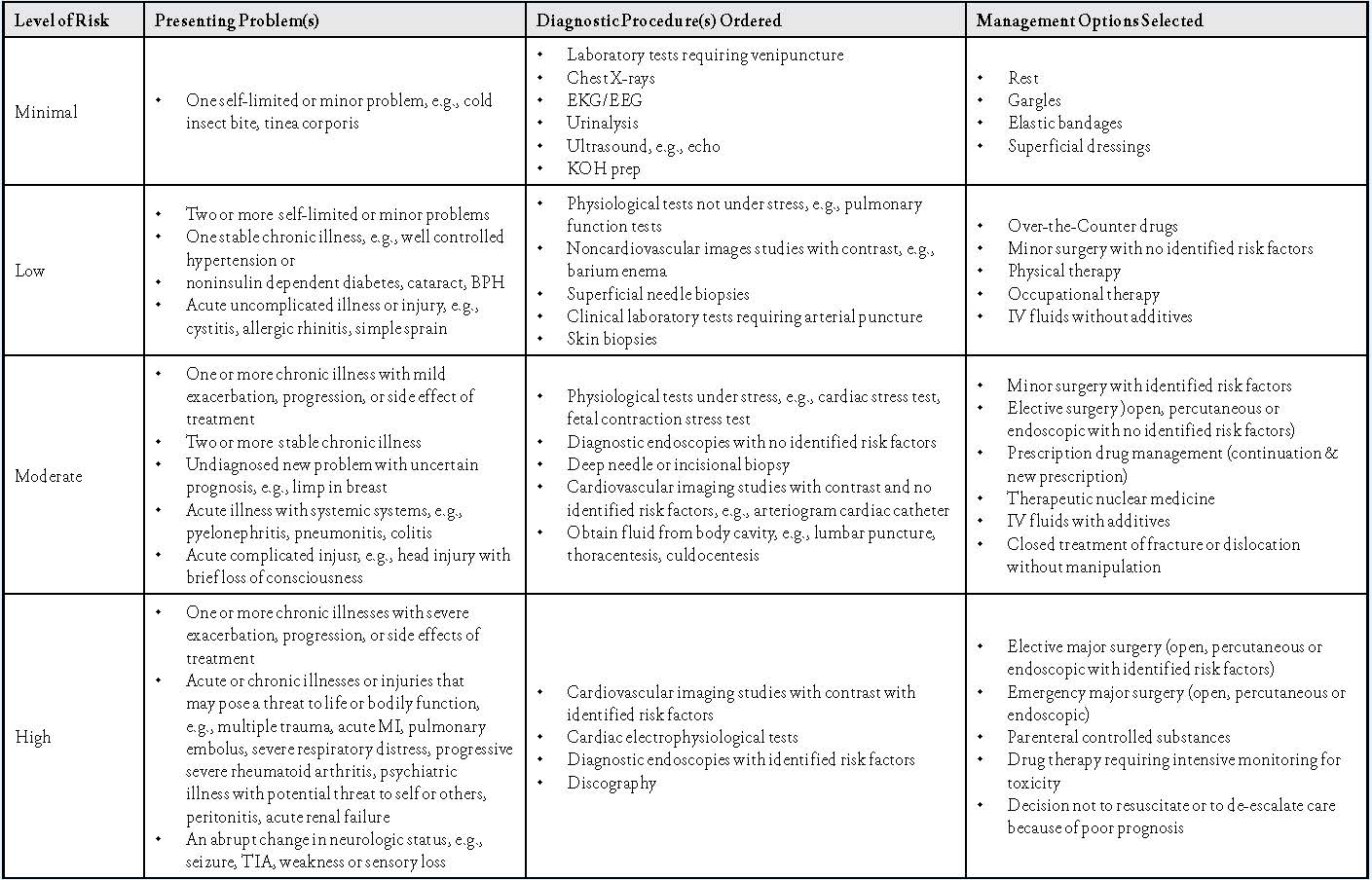
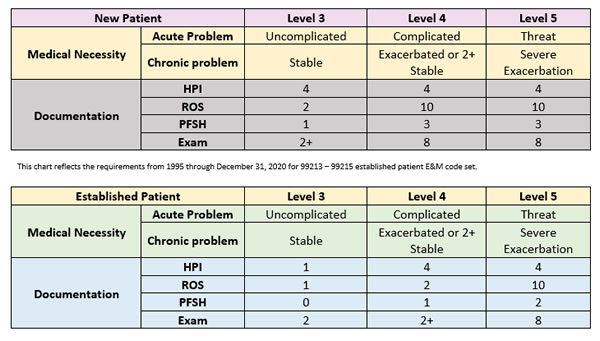
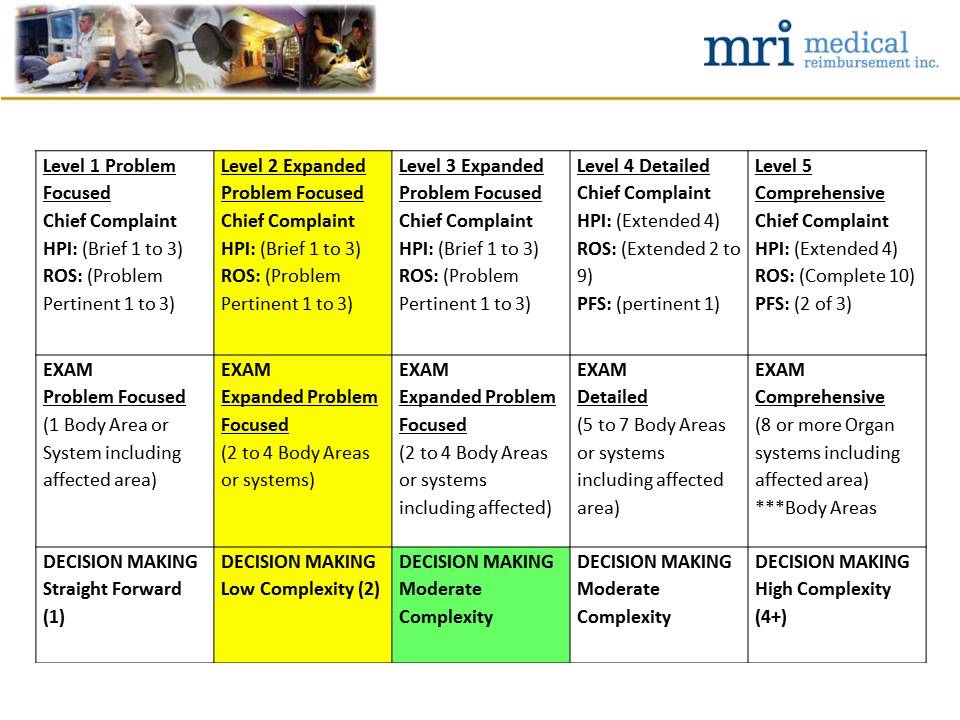
Auditor's Scoring Worksheets Using 95/97 Guidelines for Other Than Outpatient/Office E/M Services 2021 Prior to 2021 E/M Guidelines Below you will find the Documentation Guidelines that were effective prior to the 2021 Changes and those that are still in effect for Categories other than Outpatient and Office E/M codes (99202-99215)
2021 office-based E/M coding guidelines updated: 2021 office-based E/M coding guidelines updated. May 1, 2021. from the AAP Division of Health Care Finance. No.
Although the E/M interactive worksheet was created as a resource to assist providers with selecting the appropriate E/M code, it is not intended to serve as a replacement for the E/M documentation guidelines published by CMS or AMA CPT E/M Code and Guideline Changes for 2021 (effective for office/outpatient visits only for dates of service on ...
An increase in RVUs for emergency department E/M codes . In 2021, emergency medicine providers will also see changes related to the Final Rule of the Medicare Physician Fee Schedule (PFS) - including an increase in Relative Value Units (RVUs) for Emergency Department (ED) evaluation and management (E/M) codes 99283-99285.
Modified: 9/28/2021. As of July 1, 2017, practitioners in Florida are required to report post-operative evaluation and management (E/M) visits using CPT code 99024 if they practice in a group of ten or more practitioners and provide global services under one of the required surgical procedure codes.
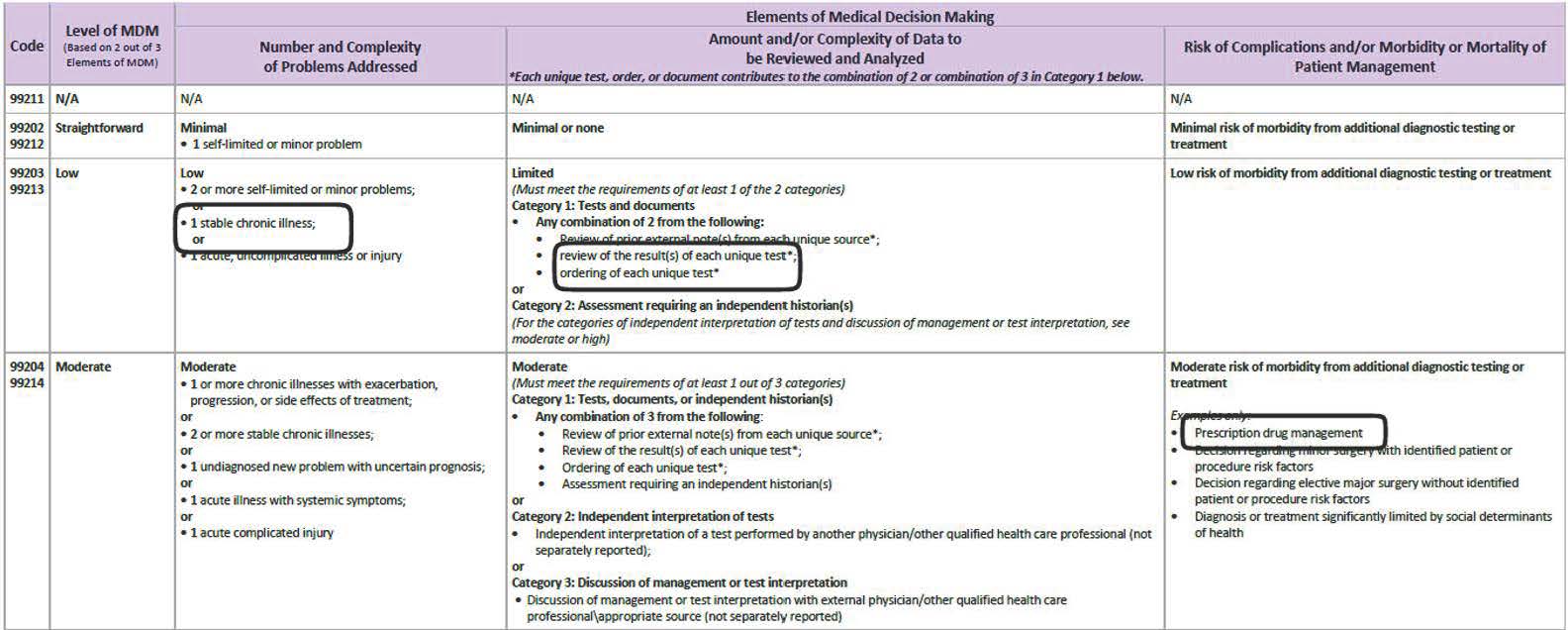
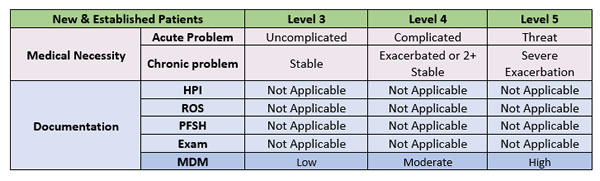
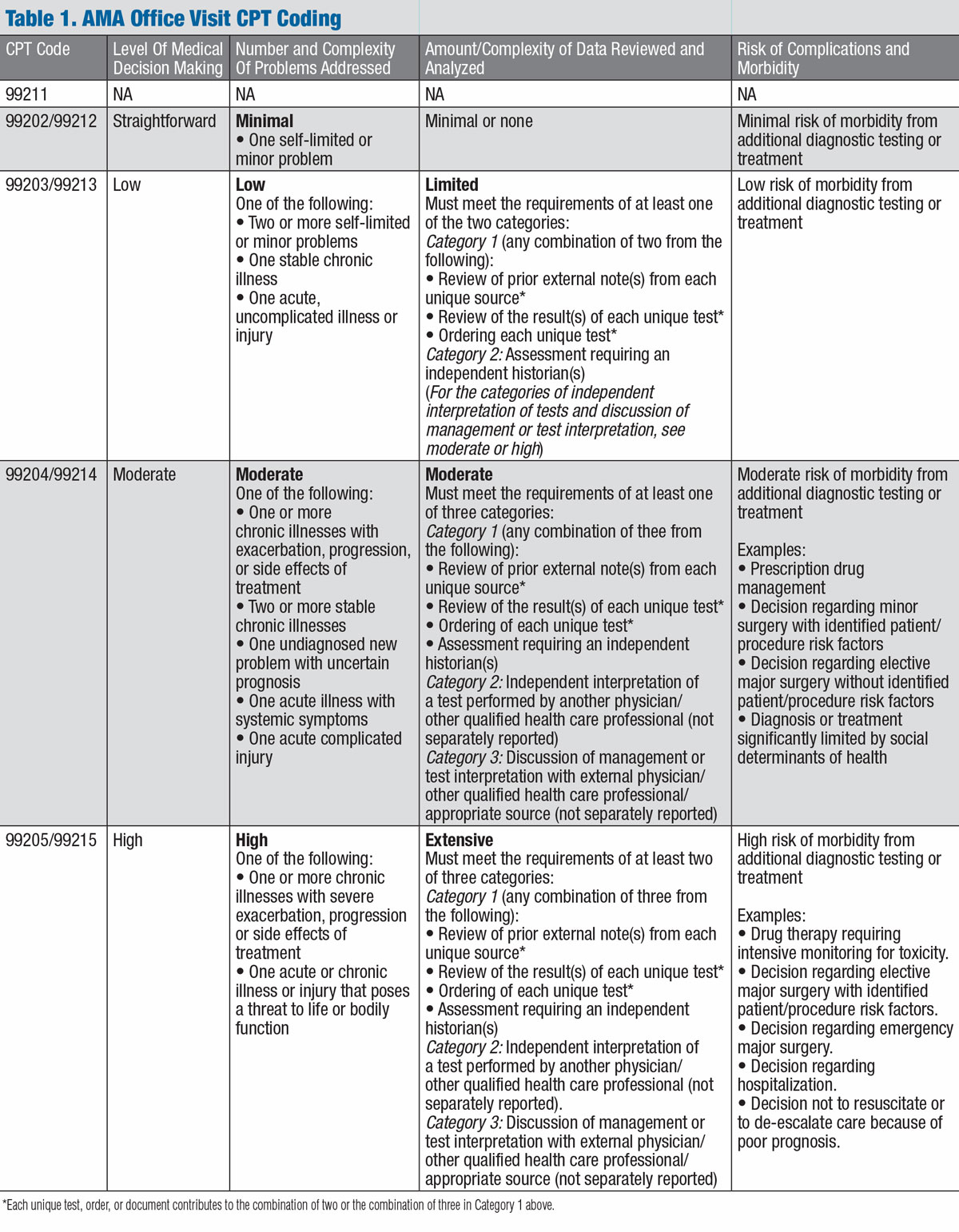
The 2021 MDM table in the CPT ® E/M guidelines has three main columns with the final column divided into three additional columns: Code Level of MDM (Based on 2 out of 3 Elements of MDM) Elements of Medical Decision Making Number and Complexity of Problems Addressed at the Encounter Amount and/or Complexity of Data to be Reviewed and Analyzed
Learn about key changes to evaluation and management (E/M) services taking place in 2021, including recent and upcoming revisions impacting E/M coding and documentation guidelines. For office/outpatient E/M visits, the 1995 and 1997 E/M guidelines will no longer be used for dates of service on and after January 1, 2021.
Office Evaluation and Management (E/M) CPT code revisions. This educational module provides an overview of the new E/M code revisions and shows how it will differ from current coding requirements and terminology. Access the Module. Once the revisions became effective on Jan. 1, 2021, the AMA received a lot of feedback on areas causing confusion.
Effective January 1, 2021, Evaluation & Management Codes for office visits have changed.E/M levels are now determined by time or a new Medical Decision Making matrix. See Downloadable PDFs below for details. For more information or to get answers to questions, visit ACOG's Payment Advocacy and Policy Portal.. 2021 Evaluation and Management Summary
Nov. 6, 2020: How 2021 E/M coding changes will reshape the physician note; Aug. 5, 2020: E/M office-visit changes on track for 2021: What doctors must know; Feb. 13, 2020: How 2021 E/M guidelines could ease physicians' documentation burdens ; Nov. 19, 2019: E/M prep: Avoid these pitfalls in move to new office-visit codes
The Academy's Conquering New E/M Documentation Guidelines for Ophthalmology provides detailed education for physicians and staff on medical decision-making and offers four hours of CME. We have also have free E/M news and advice on the Academy website. Time: One of the two elements to determine appropriate level of E/M code
This is sometimes called the "office visit" code. E&M code selection is based on medical decision making and the amount of time spent. This article collects resources and guidelines for E&M office visits, with some tips on implementation in PCC EHR. On January 1st, 2021, the guidelines for coding and billing an office visit changed ...
This E/M calculator tool was created to help identify the appropriate E/M service level. The calculator follows both CPT and Medicare coding guidelines for services prior to 2021 as well as the new guidelines effective January 1, 2021.
Coding & Billing Guidelines Emergency Department (ED) Evaluation and Management (E/M) codes are typically reported per day and do not differentiate between new or established patients. There are 5 levels of emergency department services represented by CPT codes 99281 - 99285.
by Aimee Wilcox. When Medicare determined that providers could follow EITHER the 1995 OR the 1997 Documentation Guidelines for Evaluation and Management Services to determine which level of E/M service to report, because CMS had not clarified that portions of the 1995 and 1997 guidelines could be used together to determine the level of E/M to be reported, many of the Medicare Administrative ...
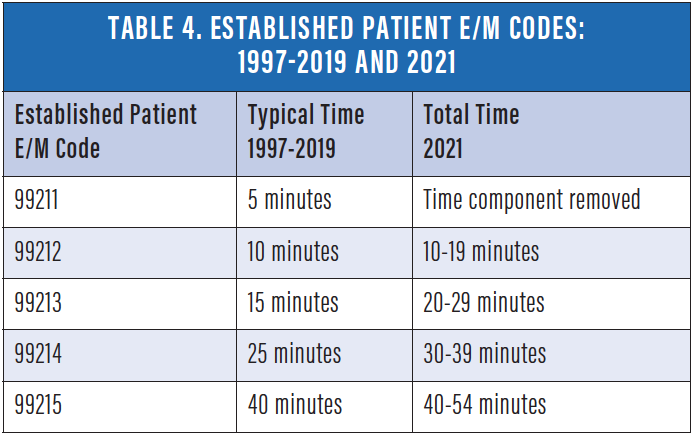
The E/M coding changes could help reduce documentation time for a few reasons. First, physicians can use simplified time increments to choose a CPT code. They no longer have to worry about confusing terms like "midpoint" or "threshold" to select the appropriate E/M code, which means they can spend less time figuring out which code to use.
CPT® Evaluation and Management (E/M) Codes. Managing E/M coding and billing is crucial for maintaining the productivity of your medical practice. Here's how the AMA is working to simplify E/M coding and reduce physician burdens. Search:
Scoring elements can be challenging with the new E/M guidelines for 2021. This article is updated based on the 5/25/2021 AMA webinar, given by Drs. Levy and Hollman. This post includes questions related to: Major/Minor procedure; Data Elements (with link to additional resources) General questions about the new guidelines
Get clarification on new E/M guidelines effective Jan. 1 from questions answered by the American Medical Association and the Academy. For more information, visi
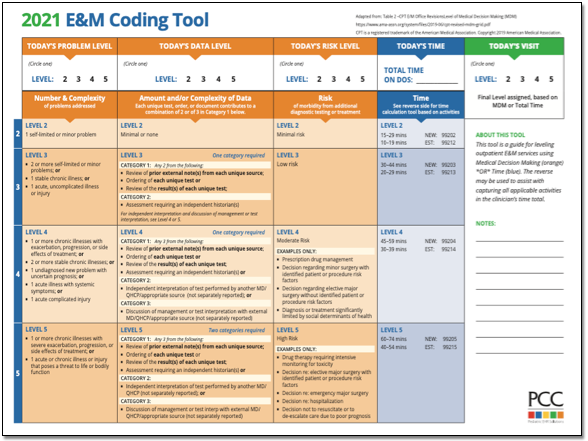
Coding Guide - E/M Changes for 2021. Do you want to be ready for the E/M changes in 2021? Download this guide for an explanation of CPT ® changes for codes 9920-99215. Learn about the new guidelines for using time to select a code and see the revised medical decision making grid. CMS is proposing to accept these AMA changes.
January 15, 2021. 2021 E/M coding and documentation rules. New rules for reporting outpatient office evaluation and management (E/M) services took effect Jan. 1. The coding and documentation revisions, adopted by the American Medical Association's CPT Editorial Panel and approved by the Centers for Medicare and Medicaid Services (CMS ...

























0 Response to "41 e/m coding guidelines worksheet"
Post a Comment